
Nutcracker Syndrome
Nutcracker Syndrome (NCS) happens when a vein that carries blood away from the left kidney gets squeezed. This can make it hard for blood to flow the right way. This most commonly happens when the left kidney vein gets squeezed between two big arteries: the aorta and the superior mesenteric artery (SMA).
- For Patients
- For Physicians
Background
Nutcracker Syndrome (NCS) happens when a vein that carries blood away from the left kidney gets squeezed. This can make it hard for blood to flow the right way. This most commonly happens when the left kidney vein gets squeezed between two big arteries: the aorta and the superior mesenteric artery (SMA). This is called anterior NCS.

Nutcracker can also happen when the vein is compressed between the aorta and the spine. This is called posterior NCS and usually happens in people whose vein takes a different path through the body (called a retro aortic vein). Some people have both types, which is called a circumaortic vein. In other words, some people have a left kidney vein that splits and goes around both sides of the aorta.

 In posterior NCS (top), the left kidney vein (LRV) is pressed between a large artery and the spine. In circumaortic NCS (bottom), the left kidney vein splits and goes around both sides of the aorta. 12 CC BY
In posterior NCS (top), the left kidney vein (LRV) is pressed between a large artery and the spine. In circumaortic NCS (bottom), the left kidney vein splits and goes around both sides of the aorta. 12 CC BYThis anatomy is called “nutcracker” because the vein looks like it’s being squished like a nut in a nutcracker.


Doctors used to think NCS did not happen very often and did not hurt the kidney; however, now we know it can cause strong pain and other symptoms.1 NCS can also make blood flow backwards in other veins, like the ones near the ovaries or testicles. This can cause bad pelvic pain.2
Some people with super flexible joints or soft tissues, like in Ehlers-Danlos syndrome (EDS), may be more likely to get NCS.3
Symptoms
- Pain in the stomach or the left side
- Blood in the urine
- Extra protein in the urine
- Swollen veins near the pelvis or genitals
- Pelvic pain or painful periods
- Tiredness and feeling dizzy
- Migraine headaches
Impact
People with NCS often have pain that does not go away. This pain can be there all the time, or it can come and go. It is estimated that about 30% of people with NCS cannot work because of how bad they feel.4
Many people with NCS take strong pain medicine like opioids. About half of NCS patients use these medicines to feel better.1
It can be hard to determine if someone has NCS. Most people see 10–15 doctors to rule out other issues before they get the right diagnosis.4
Treatments
- Compression stockings can help with pelvic pain.5
- Medicine can be taken to lower blood pressure and reduce pain.5
- Vein stents (a small tube) can be placed in the vein to keep it open (only done in patients with retro aortic vein anatomy).6
- Doctors can close off veins with soft metal coils and foam which helps stop the blood from flowing the wrong way. This procedure is called embolization and is commonly done in the gonadal vein.7
- Surgical options:
- Kidney autotransplant: The kidney is moved to another place in the body. This surgery has a 93.1% success rate.1
- Renal vein transposition: The vein is moved to stop the squeezing. This surgery improves symptoms in 87% of people, but 32% may need another treatment within 2 years.8
- Gonadal vein transposition: The vein from the ovaries or testicles is moved so blood flows better.9
- External vein stent: A stent is placed on the outside of the vein to keep it open.10
- Kidney removal: This is usually only done if nothing else works. Some people even donate the kidney to someone else.11
SAFIRE
We need to raise awareness about NCS. We also need better treatments and better insurance support. SAFIRE is raising money to study safer and easier treatments for NCS.
More doctors are learning how to treat NCS and help people with complex health problems. SAFIRE helps patients find the right doctors for their needs.
References
- Philip JL, Saben J, Meram E, et al. Renal autotransplant as a definitive treatment for nutcracker syndrome: A multicenter retrospective study. Journal of Vascular Surgery: Venous and Lymphatic Disorders.
- Zurcher KS, Staack SO, Spencer EB, et al. Venous Anatomy and Collateral Pathways of the Pelvis: An Angiographic Review. Radiographics. 2022;42(5):1532–1545.
- Sandmann W, Scholbach T, Jacobi S. Hemodynamic Consequences of Pre-and Retroaortic Left Renal Vein Compression (“Nutcracker Syndrome”) Causing a Surprising Variety of Symptoms and Complaints, Especially in Patients Affected by Hypermobility Spectrum Disorders. Journal of Vascular Surgery: Venous and Lymphatic Disorders. 2024;12(3).
- Charondo LDB, Hamouche F, Stoller M. The Journey and Barriers to Treatment of Patients With Renal Nutcracker Syndrome. Urology. 2022;169:250–255.
- de Macedo GL, Dos Santos MA, Sarris AB, Gomes RZ. Diagnosis and treatment of the Nutcracker syndrome: a review of the last 10 years. J Vasc Bras. 2018;17(3):220–228.
- Quevedo HC, Arain SA, Abi Rafeh N. Systematic review of endovascular therapy for nutcracker syndrome and case presentation. Cardiovasc Revasc Med. 2014;15(5):305–307.
- Daniels JP, Champaneria R, Shah L, Gupta JK, Birch J, Moss JG. Effectiveness of Embolization or Sclerotherapy of Pelvic Veins for Reducing Chronic Pelvic Pain: A Systematic Review. J Vasc Interv Radiol. 2016;27(10):1478–1486 e1478.
- Erben Y, Gloviczki P, Kalra M, et al. Treatment of nutcracker syndrome with open and endovascular interventions. J Vasc Surg Venous Lymphat Disord. 2015;3(4):389–396.
- Debucquois A, Salomon du Mont L, Bertho W, Kaladji A, Hartung O, Rinckenbach S. Current results of left gonadal vein transposition to treat nutcracker syndrome. J Vasc Surg Venous Lymphat Disord. 2021;9(6):1504–1509.
- Fuentes-Perez A, Bush RL, Kalra M, et al. Systematic review of endovascular versus laparoscopic extravascular stenting for treatment of nutcracker syndrome. J Vasc Surg Venous Lymphat Disord. 2023;11(2):433–441.
- Ananthan K, Onida S, Davies AH. Nutcracker Syndrome: An Update on Current Diagnostic Criteria and Management Guidelines. Eur J Vasc Endovasc Surg. 2017;53(6):886–894.
- Orczyk, Krzysztof, Wysiadecki, Grzegorz, Majos, Agata, Stefańczyk, Ludomir, Topol, Mirosław, Polguj, Michał, What Each Clinical Anatomist Has to Know about Left Renal Vein Entrapment Syndrome (Nutcracker Syndrome): A Review of the Most Important Findings, BioMed Research International, 2017, 1746570, 7 pages, 2017. https://doi.org/10.1155/2017/1746570
- Liu Y, Zheng H, Wang X, Wang Z, Zhu Q, Wen C, Tong Y. Ultrasound characteristics of abdominal vascular compression syndromes. Front Cardiovasc Med. 2023 Dec 18;10:1282597. doi: 10.3389/fcvm.2023.1282597. PMID: 38173818; PMCID: PMC10764025.
Overview
Nutcracker Syndrome (NCS) refers to compression of the left renal vein (LRV), most commonly between the superior mesenteric artery (SMA) and the aorta, referred to as anterior NCS. A less frequent variant, posterior NCS, occurs when the LRV is compressed between the aorta and the vertebral body, due to a retroaortic LRV. In some patients, both anterior and posterior compressions occur called a circumaortic LRV, where two venous branches encircle the aorta.


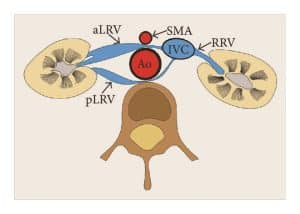
 Schematic arrangements of the main types of nutcracker syndrome. (a) Anterior type, (b) posterior type (retroaortic left renal vein), and (c) circumaortic type (circumaortic left renal vein). Ao: abdominal aorta, IVC: inferior vena cava, aLRV: anterior left renal vein, pLRV: posterior left renal vein, and SMA: superior mesenteric artery.12 CC BY
Schematic arrangements of the main types of nutcracker syndrome. (a) Anterior type, (b) posterior type (retroaortic left renal vein), and (c) circumaortic type (circumaortic left renal vein). Ao: abdominal aorta, IVC: inferior vena cava, aLRV: anterior left renal vein, pLRV: posterior left renal vein, and SMA: superior mesenteric artery.12 CC BYThe term “nutcracker” derives from the angiographic appearance of the LRV being compressed between two rigid structures, resembling a nut within a nutcracker.
Symptomatic cases of NCS are felt to be rare, but emerging data would suggest that this may be far more common than is currently recognized. Classically, nutcracker causes left flank pain and hematuria. However, recent clinical experience suggests a broad and debilitating symptom profile, including upper abdominal pain, postprandial discomfort, chest or mid-back pain, postural orthostatic tachycardia syndrome (POTS), nausea, hematuria, and flank pain.1 Emerging evidence also supports a potential overlap between NCS and autonomic dysfunction, particularly in patients with hypermobility spectrum disorders such as Ehlers-Danlos Syndrome (EDS).2 Back pain and headaches may be related in some patients as well.

Venous hypertension resulting from LRV compression often leads to collateralization of blood through the paralumbar veins/azygous, epidural venous plexus, diaphragmatic veins, or retroperitoneal veins felt to cause above symptoms or more classically retrograde into the gonadal vein reflux, manifesting with significant chronic pelvic pain.3
Clinical Presentation
- Chronic abdominal and left flank pain
- Microscopic or gross hematuria
- Proteinuria
- Pelvic varicosities and genital vein engorgement
- Dysmenorrhea and chronic pelvic pain
- Fatigue
- Orthostatic intolerance, including POTS
- Left chest pain
- Migraine headaches
- Food fear, nausea, and vomiting
Impact
NCS often presents with debilitating, refractory pain. The condition is underdiagnosed, with patients frequently consulting 10–15 healthcare providers to rule out other conditions before definitive diagnosis.4 Approximately 30% of affected patients are functionally disabled and unable to maintain employment.4 Opioid dependence is common, with up to 50% of patients requiring long-term opioid analgesia.1
Management Options
Conservative Management5
Indicated for patients with mild or intermittent symptoms. Interventions include:
- Compression stockings for pelvic pain symptoms
- Antihypertensive or neuropathic pain medications
Endovascular Interventions
- LRV stenting: Intravenous deployment of a stent to relieve compression6 Due to high rates and rare cases of vascular erosion as well as not having ideal stents for the renal vein available this has been reserved for retro aortic renal veins.
- Gonadal vein embolization: Embolization using coils and/or sclerosing agents to treat reflux from venous hypertension7
Surgical Interventions
- Renal autotransplantation: Autologous kidney relocation to the iliac fossa to relieve LRV obstruction has gained traction as the often preferred method of treatment. This surgery has shown symptom relief in 93.1% of patients in a multicenter study with low complication rates.1
- LRV transposition: Mobilization and reimplantation of the LRV into the IVC, bypassing the compression point. This surgery has been shown to alleviate symptoms in 87% of cases, though 32% may require reintervention within 2 years.8
- Left gonadal vein transposition: Rerouting the gonadal vein directly into the iliac system to decompress pelvic collaterals, create a natural bypass from the compression, and alleviate symptoms associated with pelvic venous hypertension secondary to NCS.9
- Extravascular stenting: Surgical application of an external stent around the LRV to prevent collapse, particularly during dynamic movement or postural changes.10 These have been shown to be effective but stent migration and bleeding complication requiring removal of the kidney, as well as persistent compression requiring internal stenting with subsequent stent migration have been described.
- Nephrectomy: For patients with intractable symptoms after exhausting less invasive modalities and/or high risk for reimplantation, removal of the kidney can be a good option. It is possible for patients in this situation to consider donation of their kidney which may have a positive emotional impact as well from one chronically ill patient helping another.11
SAFIRE Initiative
There is an unmet need for greater diagnostic awareness, standardized treatment protocols, and payer reform for Nutcracker Syndrome. SAFIRE is supporting clinical research focused on developing minimally invasive, durable treatment modalities and fostering interdisciplinary care networks. Our platform connects patients with experienced specialists who can provide targeted, evidence-informed care.
If you are interested in supporting SAFIRE’s mission, please consider making a contribution through our donation page.
References
- Philip JL, Saben J, Meram E, et al. Renal autotransplant as a definitive treatment for nutcracker syndrome: A multicenter retrospective study. Journal of Vascular Surgery: Venous and Lymphatic Disorders.
- Sandmann W, Scholbach T, Jacobi S. Hemodynamic Consequences of Pre-and Retroaortic Left Renal Vein Compression (“Nutcracker Syndrome”) Causing a Surprising Variety of Symptoms and Complaints, Especially in Patients Affected by Hypermobility Spectrum Disorders. Journal of Vascular Surgery: Venous and Lymphatic Disorders. 2024;12(3).
- Zurcher KS, Staack SO, Spencer EB, et al. Venous Anatomy and Collateral Pathways of the Pelvis: An Angiographic Review. Radiographics. 2022;42(5):1532–1545.
- Charondo LDB, Hamouche F, Stoller M. The Journey and Barriers to Treatment of Patients With Renal Nutcracker Syndrome. Urology. 2022;169:250–255.
- de Macedo GL, Dos Santos MA, Sarris AB, Gomes RZ. Diagnosis and treatment of the Nutcracker syndrome: a review of the last 10 years. J Vasc Bras. 2018;17(3):220–228.
- Quevedo HC, Arain SA, Abi Rafeh N. Systematic review of endovascular therapy for nutcracker syndrome and case presentation. Cardiovasc Revasc Med. 2014;15(5):305–307.
- Daniels JP, Champaneria R, Shah L, Gupta JK, Birch J, Moss JG. Effectiveness of Embolization or Sclerotherapy of Pelvic Veins for Reducing Chronic Pelvic Pain: A Systematic Review. J Vasc Interv Radiol. 2016;27(10):1478–1486 e1478.
- Erben Y, Gloviczki P, Kalra M, et al. Treatment of nutcracker syndrome with open and endovascular interventions. J Vasc Surg Venous Lymphat Disord. 2015;3(4):389–396.
- Debucquois A, Salomon du Mont L, Bertho W, Kaladji A, Hartung O, Rinckenbach S. Current results of left gonadal vein transposition to treat nutcracker syndrome. J Vasc Surg Venous Lymphat Disord. 2021;9(6):1504–1509.
- Fuentes-Perez A, Bush RL, Kalra M, et al. Systematic review of endovascular versus laparoscopic extravascular stenting for treatment of nutcracker syndrome. J Vasc Surg Venous Lymphat Disord. 2023;11(2):433–441.
- Ananthan K, Onida S, Davies AH. Nutcracker Syndrome: An Update on Current Diagnostic Criteria and Management Guidelines. Eur J Vasc Endovasc Surg. 2017;53(6):886–894.
- Orczyk, Krzysztof, Wysiadecki, Grzegorz, Majos, Agata, Stefańczyk, Ludomir, Topol, Mirosław, Polguj, Michał, What Each Clinical Anatomist Has to Know about Left Renal Vein Entrapment Syndrome (Nutcracker Syndrome): A Review of the Most Important Findings, BioMed Research International, 2017, 1746570, 7 pages, 2017. https://doi.org/10.1155/2017/1746570
- Liu Y, Zheng H, Wang X, Wang Z, Zhu Q, Wen C, Tong Y. Ultrasound characteristics of abdominal vascular compression syndromes. Front Cardiovasc Med. 2023 Dec 18;10:1282597. doi: 10.3389/fcvm.2023.1282597. PMID: 38173818; PMCID: PMC10764025.