Deep Vein Thrombosis (DVT)
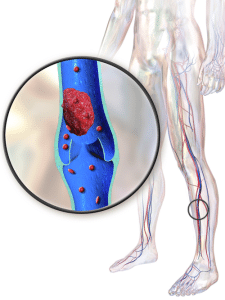
Deep vein thrombosis, or DVT, happens when a blood clot forms in a deep vein—typically in the leg.1 Blood clots are clumps of blood that have turned solid. This can be dangerous because if the clot moves, it can travel to the lungs and cause a serious problem called a pulmonary embolism (PE).
- For Patients
- For Physicians
What Is It?
Deep vein thrombosis, or DVT, happens when a blood clot forms in a deep vein—typically in the leg.1 Blood clots are clumps of blood that have turned solid. This can be dangerous because if the clot moves, it can travel to the lungs and cause a serious problem called a pulmonary embolism (PE).
Both DVT and PE are encompassed by the term venous thromboembolism (VTE). The three leading causes of cardiovascular death in the world in order are (1) heart attack, (2) stroke, and (3) VTE.2,3
How Common Is It?
A study looked at over 21,000 people who were 45 years old or older and followed them for over 7 years. They found that for every 1,000 people, approximately 1.92 people had a first-time VTE each year. In this study, the rate of VTE increased with age and was higher in men compared to women.4
Types of DVT
Doctors group DVT into three types depending on how long the clot has been there. The classifications are based on either the duration of symptoms the patient has experienced or the time that has lapsed since the clot first formed, as determined by image review. DVTs are then grouped into the following categories:5
- Acute DVT: less than 14 days old
- Subacute DVT: 15 to 28 days old
- Chronic DVT: more than 28 days old
What Makes Someone More Likely to Get DVT?
Here are some things that may raise your chances of having a DVT:2,5
- Prior history of DVT
- Surgery or injury
- Not moving for a long time (e.g., extended hospitalization or being on a long trip)
- Cancer
- Blood clotting abnormality
- Being pregnant or recently giving birth
- Taking hormones (like birth control or hormone therapy)
- Smoking
- Being overweight
Signs and Symptoms
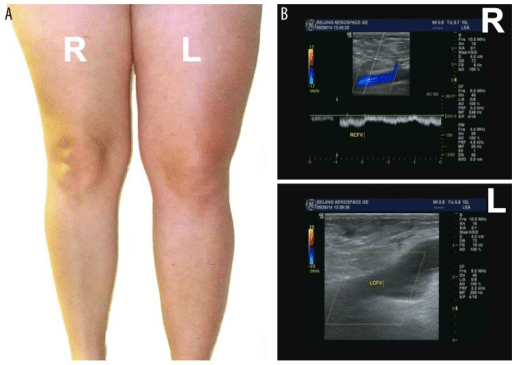
People with DVT in their legs may experience the following:2,3
- Pain in the leg
- Swelling
- Red skin
- Changes in how the skin looks
- Sores, or ulcers, on the skin
- Varicose veins or bulging veins
- The leg feeling hot
Impact
DVT can affect a person’s daily life and have lasting effects. Even after treatment, some people have long-term problems, like:
- Post-thrombotic syndrome: Pain, swelling, or skin problems from vein damage (this happens to about 43% of patients, and 3% have severe symptoms).3
- Recurrent DVT: Studies have shown that as many as 1 in 4 people may get DVT again.3
How Do Doctors Find Out If You Have DVT?
There are a few ways that healthcare providers may evaluate for DVT. These may include any of the following: 3,5-9
- Wells score: A checklist that helps doctors evaluate how likely it is that you have a DVT
- D-dimer test: A blood test that shows if there might be a clot by measuring something called a “D-dimer”. A D-dimer is a protein fragment that is produced when blood clots break down in the body. Having a high D-dimer level may indicate that a clot is present and warrants further testing.
- Imaging: can be used to further evaluate and confirm the presence of DVT
- Ultrasound
- CT venogram
- MR venography
How Is DVT Treated?
There are many ways to treat DVT, depending on how serious it is:
- Compression stockings: Stockings that fit tighter than normal socks, which help to improve blood flow
- Blood thinners: Medication that helps to break up the clot and stop new ones from forming
- Thrombectomy: A procedure to remove the clot from the vein
- Thrombolysis: A thrombolytic is a medication that helps dissolve a clot. Years ago, thrombolysis was done by giving a thrombolytic by systemic infusion (or to the entire body). However, direct administration of the thrombolytic into the clot has been shown to accelerate thrombolysis.10
- Catheter-directed thrombolysis (CDT): CDT is performed by administering thrombolytic medication directly into or at the site of the clot. This is done by using a specialty catheter with multiple side-holes that allows the medication to be released to a specific area.10
- Ultrasound accelerated thrombolysis (USAT): In recent years, USAT (a new CDT technique) has been shown to decrease the time it takes to dissolve the clot and improve outcomes. The ACCESS PTS trial showed significant improvement in chronic DVT patients after angioplasty and thrombolysis with EKOS using recombinant tissue-type plasminogen activator.11
While there are good treatments for acute and even subacute DVT currently, chronic DVT or prolonged scarring/blockages in the veins can lead to advanced skin changes, pain, and swelling in the lower extremities. Reconstruction techniques can improve symptoms but are rarely offered and are challenging to perform. Chronic DVT reconstruction is a field that will benefit from further study and education for both providers and patients.
What Is SAFIRE Doing to Help?
SAFIRE aims to restore hope in patients affected by chronic DVT by:
- Advancing research on chronic DVT and treatment options by funding research projects
- Exploring the link between DVT and pelvic venous disorders
- Providing educational resources to both patients and healthcare professionals
- Improving access to care by creating a network of providers, including providers that specialize in the diagnosis and treatment of DVT
If you are interested in supporting SAFIRE’s mission, please consider contributing through our donation page.
References
- Navarrete S, Solar C, Tapia R, Pereira J, Fuentes E, Palomo I. Pathophysiology of deep vein thrombosis. Clin Exp Med. 2023;23(3):645–654.
- Wolberg AS, Rosendaal FR, Weitz JI, et al. Venous thrombosis. Nat Rev Dis Primers. 2015;1:15006.
- Waheed SM, Kudaravalli P, Hotwagner DT. Deep Vein Thrombosis. In: StatPearls. Treasure Island FL ineligible companies. Disclosure: Pujitha Kudaravalli declares no relevant financial relationships with ineligible companies. Disclosure: David Hotwagner declares no relevant financial relationships with ineligible companies.: © 2025, StatPearls Publishing LLC.; 2025.
- Cushman M, Tsai AW, White RH, et al. Deep vein thrombosis and pulmonary embolism in two cohorts: the longitudinal investigation of thromboembolism etiology. Am J Med. 2004;117(1):19–25.
- Vedantham S, Grassi CJ, Ferral H, et al. Reporting standards for endovascular treatment of lower extremity deep vein thrombosis. J Vasc Interv Radiol. 2009;20(7 Suppl):S391–408.
- Karande GY, Hedgire SS, Sanchez Y, et al. Advanced imaging in acute and chronic deep vein thrombosis. Cardiovasc Diagn Ther. 2016;6(6):493–507.
- Library CCsH. Venogram. 2023; https://my.clevelandclinic.org/health/diagnostics/24929-venogram. Accessed 24Feb2025.
- Usman S, Cheema M, Mustafa S, et al. Pulse Wave Doppler Ultrasound in Unmasking of Venous Obstructions Highlighting Diagnostic Utility and Clinical Implications. J Intensive Care Med. 2025;40(1):109–116.
- Hudgens SA, Cella D, Caprini CA, Caprini JA. Deep vein thrombosis: validation of a patient-reported leg symptom index. Health Qual Life Outcomes. 2003;1:76.
- Kim KA, Choi SY, Kim R. Endovascular Treatment for Lower Extremity Deep Vein Thrombosis: An Overview. Korean J Radiol. 2021;22(6):931–943.
- Garcia MJ, Sterling KM, Kahn SR, et al. Ultrasound-Accelerated Thrombolysis and Venoplasty for the Treatment of the Postthrombotic Syndrome: Results of the ACCESS PTS Study. J Am Heart Assoc. 2020;9(3):e013398.
- Blausen.com staff (2014). “Medical gallery of Blausen Medical 2014”. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436
- Li Y, Guan XH, Wang R, et al. Active Ankle Movements Prevent Formation of Lower-Extremity Deep Venous Thrombosis After Orthopedic Surgery. Med Sci Monit. 2016;22:3169-3176. Published 2016 Sep 7. doi:10.12659/msm.896911
Background
Deep vein thrombosis (DVT) is a multifactorial thrombotic condition involving the formation of fibrin-rich thrombi within the deep venous system, most commonly of the lower extremities.1 Thrombi in these vessels may embolize and migrate to the lungs, resulting in pulmonary embolism (PE). Together, DVT and PE are referred to as venous thromboembolism (VTE), which ranks as the third most common cause of cardiovascular mortality globally, following myocardial infarction and cerebrovascular accidents.2,3
Epidemiological data from a cohort of 21,680 individuals aged ≥45 years, followed longitudinally for over 7 years, indicate an age-standardized incidence of first VTE at 1.92 per 1,000 person-years. Incidence was positively correlated with age and demonstrated a higher prevalence in males compared to females.4
The Journal of Vascular and Interventional Radiology classifies DVT temporally based on duration of symptoms or thrombus age confirmed via imaging:5
- Acute: ≤14 days
- Subacute: 15–28 days
- Chronic: >28 days

Risk Factors
Predisposing factors for DVT may include:2,5
- Personal or family history of DVT
- Recent surgery or trauma
- Prolonged immobility (e.g., hospitalization, long-haul travel)
- Malignancy
- Inherited or acquired coagulation abnormality
- Pregnancy and the postpartum period
- Hormonal therapy (e.g., oral contraceptives, HRT)
- Tobacco use
- Obesity
Clinical Presentation
Signs and symptoms of lower extremity DVT may include:2,3
- Leg pain
- Leg swelling
- Erythema
- Increased warmth
- Skin changes
- Ulceration
- Varicose veins
Complications and Long-term Impact
Although many patients experience symptom resolution with anticoagulation, long-term sequelae are common and may significantly impair quality of life. Key complications include:
- Post-thrombotic syndrome (PTS): Characterized by chronic venous insufficiency symptoms (e.g., pain, edema, skin changes), PTS occurs in approximately 43% of patients at 2 years post-DVT, with 3% experiencing severe symptoms.3
- Recurrent DVT: Risk of recurrence has been shown to be as high as 25%.3
Diagnostic Evaluation
The diagnostic workup for suspected DVT incorporates both clinical decision rules and confirmatory testing:3,5-9
- Wells Criteria: Assesses pre-test probability (low, moderate, high)
- D-dimer assay: Useful for ruling out DVT in low to moderate risk patients due to high negative predictive value
- Imaging modalities:
- Duplex ultrasonography: First-line for proximal DVT; high sensitivity and specificity
- CT venography or MR venography: Employed in complex or inconclusive cases, or when pelvic/abdominal vein involvement is suspected

Management Strategies
Treatment is guided by clot location, symptom duration, risk stratification, and patient-specific factors. Options include:
- Compression therapy: Compression stockings improve venous return and may reduce PTS risk
- Anticoagulation: Direct oral anticoagulants (DOACs), low molecular weight heparin (LMWH), or warfarin, depending on indication and comorbidities
- Thrombectomy: A procedure during which the thrombus is removed from the vein
- Thrombolysis: Years ago, thrombolysis was performed by administering a thrombolytic agent by systemic infusion; however, direct administration of thrombolytics into the thrombus has been shown to accelerate thrombolysis.10
- Catheter-directed thrombolysis (CDT): CDT is performed by administering a thrombolytic agent directly into or at the site of the thrombus via a specialty catheter with multiple side-holes.10
- Ultrasound accelerated thrombolysis (USAT): In recent years, USAT (a new CDT technique) has been shown to decrease the time to dissolution of thrombus and increase clinical improvements. The ACCESS PTS trial showed significant improvement in chronic DVT patients after angioplasty and thrombolysis with EKOS using recombinant tissue-type plasminogen activator.11
While there are good treatments for acute and even subacute DVT currently, chronic DVT or prolonged scarring/blockages in the veins can lead to advanced skin changes, pain, and swelling in the lower extremities. Reconstruction techniques with stenting and balloon angioplasty of the lower extremities can improve symptoms but are rarely offered and are technically challenging. Chronic DVT reconstruction is a field that will benefit from further study and education for both providers and patients.
SAFIRE’s Role in Advancing Care
The SAFIRE initiative seeks to address the unmet needs of patients with chronic DVT through a multi-pronged approach:
- Advancing research on chronic DVT and treatment options by funding research projects
- Exploring the link between DVT and pelvic venous disorders
- Providing educational resources to both patients and healthcare professionals
- Improving access to care by creating a network of providers, including providers that specialize in the diagnosis and treatment of DVT
If you are interested in supporting SAFIRE’s mission, please consider contributing through our donation page.
References
- Navarrete S, Solar C, Tapia R, Pereira J, Fuentes E, Palomo I. Pathophysiology of deep vein thrombosis. Clin Exp Med. 2023;23(3):645–654.
- Wolberg AS, Rosendaal FR, Weitz JI, et al. Venous thrombosis. Nat Rev Dis Primers. 2015;1:15006.
- Waheed SM, Kudaravalli P, Hotwagner DT. Deep Vein Thrombosis. In: StatPearls. Treasure Island FL ineligible companies. Disclosure: Pujitha Kudaravalli declares no relevant financial relationships with ineligible companies. Disclosure: David Hotwagner declares no relevant financial relationships with ineligible companies.: © 2025, StatPearls Publishing LLC.; 2025.
- Cushman M, Tsai AW, White RH, et al. Deep vein thrombosis and pulmonary embolism in two cohorts: the longitudinal investigation of thromboembolism etiology. Am J Med. 2004;117(1):19–25.
- Vedantham S, Grassi CJ, Ferral H, et al. Reporting standards for endovascular treatment of lower extremity deep vein thrombosis. J Vasc Interv Radiol. 2009;20(7 Suppl):S391–408.
- Karande GY, Hedgire SS, Sanchez Y, et al. Advanced imaging in acute and chronic deep vein thrombosis. Cardiovasc Diagn Ther. 2016;6(6):493–507.
- Library CCsH. Venogram. 2023; https://my.clevelandclinic.org/health/diagnostics/24929-venogram. Accessed 24Feb2025.
- Usman S, Cheema M, Mustafa S, et al. Pulse Wave Doppler Ultrasound in Unmasking of Venous Obstructions Highlighting Diagnostic Utility and Clinical Implications. J Intensive Care Med. 2025;40(1):109–116.
- Hudgens SA, Cella D, Caprini CA, Caprini JA. Deep vein thrombosis: validation of a patient-reported leg symptom index. Health Qual Life Outcomes. 2003;1:76.
- Kim KA, Choi SY, Kim R. Endovascular Treatment for Lower Extremity Deep Vein Thrombosis: An Overview. Korean J Radiol. 2021;22(6):931–943.
- Garcia MJ, Sterling KM, Kahn SR, et al. Ultrasound-Accelerated Thrombolysis and Venoplasty for the Treatment of the Postthrombotic Syndrome: Results of the ACCESS PTS Study. J Am Heart Assoc. 2020;9(3):e013398.
- Memtsas, Vassilios & Arachchillage, Deepa & Gorog, Diana. (2021). Role, Laboratory Assessment and Clinical Relevance of Fibrin, Factor XIII and Endogenous Fibrinolysis in Arterial and Venous Thrombosis. International Journal of Molecular Sciences. 22. 1472. 10.3390/ijms22031472.
- Li Y, Guan XH, Wang R, et al. Active Ankle Movements Prevent Formation of Lower-Extremity Deep Venous Thrombosis After Orthopedic Surgery. Med Sci Monit. 2016;22:3169-3176. Published 2016 Sep 7. doi:10.12659/msm.896911